Aspirin and Heart Disease Prevention

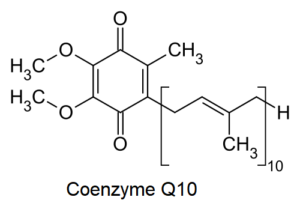
Aspirin is a derivative of salicylic acid, a compound found in willow bark, meadowsweet and other herbal plant species. Early on, salicylic acid was recognized as one of the main, active ingredients in these plants that helped treat fever and pain. However, due to it’s acrid taste and irritating nature, salicylic acid wasn’t widely adopted as medicine. In the late 1800s, a chemist who worked at Friedrich Bayer and Company, rediscovered an earlier process on how to add an “acetyl” group to salicylic acid. The improved profile of the chemical, acetylsalicylic acid, became what we know of today as aspirin. Initially sold as a powder, then produced as a tablet, aspirin launched the pharmaceutical industry (Rinsema 1999).
Aspirin as a Blood Thinner
In the first half of the 20th century, tonsillectomy was often treated with aspirin containing chewing gum to help reduce pain and inflammation. Unfortunately, doses of aspirin were so high that it wasn’t uncommon for patients to have bleeding events. In 1950, a doctor noting the increased bleeding from high-dose aspirin use, hypothesized that aspirin might be useful to decrease clotting and prevent heart disease. Laurence Craven, a physician in California, started prescribing aspirin to prevent heart attack and stroke in older individuals based on his initial observations (Miner 2007). Initially, Craven reported on 400 patients that he treated with aspirin with no heart attacks. He then went on to treat 8000 patients and further claimed prevention of heart attack and stroke (Craven 1956).
For many years, Craven’s studies were mostly ignored. While a separate anticoagulant, dicumarol, was often prescribed for heart attacks, significant controversy remained about antithrombotic (anticlotting) agents and heart disease (Wright 1945). Still, it wasn’t until 1971 that researchers were able to tease out the mechanisms of how aspirin affects platelets reducing their propensity to clot (Vane 1971).
With this understanding large clinical trials reporting benefits for treating heart disease and stroke with aspirin began to emerge (Elwood 1974, CDPRG 1976). Arguably, one of the most important discoveries was the benefits from aspirin given at the beginning of a heart attack. Aspirin, administered early, was found to significantly help open clogged blood vessels and improve clinical outcomes (ISIS 1989). At the first sign of a heart attack, chewing and swallowing 162-325 mg of aspirin is recommended to improve outcomes (Berger 2008).
Aspirin for Primary Prevention of Heart Attack and Stroke
Aspirin has become a common recommendation to help prevent heart attacks and strokes in healthy individuals. I commonly see baby aspirin included in patient’s medication lists. Yet in patients with no history of heart attack or stroke, the common recommendation for aspirin may deserve questioning in light of the latest clinical trials.
One of the larger recent studies involved almost 20,000 patients aged 70 and older without dementia, heart disease or disability. Half of the participants were given 100 mg of aspirin and half placebo. The study found a small, but higher risk of death in those given aspirin. The main cause of increased death was due to cancer (McNeil 2018). The results are particularly surprising in light of the fact that heart disease and stroke are leading causes of death which aspirin is supposed to help prevent. However, other recent studies on aspirin for primary prevention of heart attacks have also found lack of benefit (Gaziano 2018).
While these studies are likely not the last word on using aspirin in healthy individuals to prevent heart attack and stroke, it’s worth asking serious questions about the validity of its use. Other meta-analyses have still argued for benefits. One analysis highlighted a decrease in cardiovascular events, at a cost of increased bleeding (Barabarawi 2019). Death rates with aspirin were unchanged. I might argue that trading severe heart events for severe bleeding episodes is not an effective treatment strategy.
It also needs to be strongly emphasized that these studies were exploring what is called primary prevention. Primary prevention is an attempt to prevent a disease in an individual with no prior history of the condition. Aspirin use for secondary prevention of heart attacks and stroke has stronger evidence. However, caveats still exist in some of the latest research.
Aspirin and Secondary Prevention
Based on what we know, it would be negligent of me to claim that low-dose aspirin has no place in disease prevention. Research on secondary prevention, using aspirin for preventing a second heart attack or stroke is robust, especially for the first year following the event. However, after that year, benefits appear to taper off. Continued use of aspirin for secondary prevention after a year needs more evaluation. The American College of Cardiology currently recommends continued lifelong low-dose aspirin for secondary prevention, although they also advocate for additional research to better understand the best approach (Hsu 2013, Jacobsen 2020).
Aspirin and Safety
Over-the-counter aspirin has been around for a long-time, available in stores without a prescription. Most people think of aspirin as a safe medication. However, aspirin, even in low-dose, can cause problems including:
- Bleeding problems in general
- Gastrointestinal ulcers and bleeding, which can be severe
- Allergic reactions, which can be life threatening
- Kidney toxicity
- Increased uric acid (potentially worsening gout)
Aspirin use increases gastrointestinal bleeding events and complications by 60% (Thorat 2015). As patients get older, especially after age 70, aspirin-induced fatalities increase. In addition, aspirin, even in low-dose, can affect kidney function in as little as one week in elderly individuals (Caspi 2000).
Reye syndrome, although rare, can still affect children as well. Aspirin used to treat a fever during a viral infection in children can cause liver and brain swelling. This can progress to confusion, seizures and loss of consciousness. Children and teenagers in general, should avoid aspirin use for fever, chicken pox and flu.
Conclusion
Aspirin is a fascinating medicine with a long history of use in the United States. In patients without a history of heart attack or stroke, using aspirin for prevention may not be the best course of action. Even after more than one hundred years of research, we’re still teasing out the best approach to its use.