Integrative Approaches for Heartburn Relief

Heartburn is a common problem caused by acid reflux. In severe cases, when the problem becomes chronic, gastroesophageal reflux disease (GERD) can develop. Over time, stomach acid repeatedly making its way up the throat can cause serious damage. This can lead to cancer for a small subset of individuals.
So what leads to heartburn and what strategies are effective for treatment? The incidence of GERD has been increasing. Estimates suggest around one in five adults struggles with the condition (El-Serag 2014). I can vouch for this personally, as prescriptions for proton pump inhibitors that block stomach acid production are extremely common in patients I’ve worked with.
Physiology of GERD
Hiatal Hernia
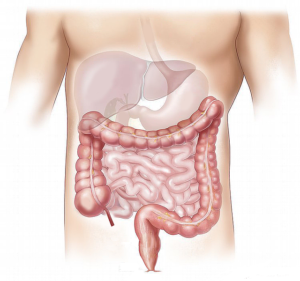
When you swallow food, it travels from the back of the throat, down the esophagus, and into the stomach. At the lower end, just before the stomach, the esophagus passes through the diaphragm. A hiatal hernia is when the stomach slips upwards through the opening in the diaphragm towards the throat.
Normally, the sphincter at the base of the esophagus and the diaphragm line up and function together to close off the stomach. With a hernia, they no longer line up and closure of the stomach can be compromised (Kahrilas 1999). It is well documented that patients with hiatal hernia are at increased risk for acid reflux (van Herwaarden 2000).
A hiatal hernia also creates an “acid pocket” or “acid film” at the top of the stomach. When a hernia is present, food doesn’t mix as well in the upper stomach. As stomach contents rise with a meal, this acid can extend into the throat, causing symptoms of heartburn (Pandolfino 2007).
Lower Esophageal Sphincter Dysfunction
As previously mentioned, at the base of the esophagus, just before the stomach, is a circular band of muscle that can help close off the throat. This band of muscle is referred to as the lower esophageal sphincter (LES). Normally, the diaphragm and the sphincter at the bottom of the esophagus work together to help seal the stomach. When the stomach contains food, pressure from the LES increases, helping to block stomach contents entering the throat.
Recent research has also highlighted that the strength and duration of LES contraction can play a role in GERD and acid reflux. When the muscle doesn’t contract well, the sphincter is not as effective at keeping stomach contents where they belong.
In patients suffering with GERD, both hiatal hernia and functional problems with the LES appear to play into the severity of the condition (Hoshino 2011).
Treatments for Acid Reflux
Conventional Treatment
Conventional approaches for relief use acid blockers, medications that decrease the production of stomach acid. While this can stop the irritation of the throat from acid reflux, it can cause problems with digestion. There’s a reason the stomach is acidic, it helps kill bacteria present on food and assists with digestion.
Some of the latest research is starting to suggest that these medications come with significant long-term risks. They appear to increase risks for bone fractures (Briganti 2021). Acid blockers also increase risk for eczema, or atopic dermatitis (Lin 2021). Other research suggests potential increased risks for pneumonia, gastrointestinal infections, nutritional deficiencies, including low magnesium and vitamin B12, kidney disease and dementia (Nehra 2018). When possible, it’s probably advisable to try and avoid long term use of acid blocking medication.
Integrative Approaches
There are other approaches to treating heartburn and acid reflux. Some of the more promising are outlined below.
Diet

Diet has a clear association with risks for acid reflux. Foods that may exacerbate symptoms include, acidic foods, carbonated beverages, chocolate, alcohol, coffee, fried foods and spicy foods. Reduction in sugar and refined carbohydrates can help reduce reflux. Increasing fiber can also be key. Decreasing meal size and not eating close to bedtime are also important components of dietary treatment (Newberry 2019).
Deglycyrrhizinated Licorice (DGL)
DGL is a soothing demulcent that can help decrease inflammation. It appears to help treat a number of gastrointestinal complaints, including heartburn (Raveendra 2012). When using licorice for digestive complaints, you typically want the deglycyrrhizinated form. Whole licorice carries risks for elevated blood pressure due to loss of potassium. The deglycyrrhizinated form should eliminate these risks.
Iberogast
Iberogast is an alcoholic herbal extract with a history of use for gastrointestinal complaints. Research shows consistent benefits in functional dyspepsia and irritable bowel syndrome. Reflux is often a component of functional dyspepsia. In addition, Iberogast has a solid safety profile with minimal side effects (Lapina 2017).
Melatonin
While usually just considered a sleep aid, melatonin has a profound impact on overall health, including gastrointestinal disorders (Munjal 2018). Research has shown significant benefits in irritable bowel syndrome and studies also appear to show promise in treating GERD.
Keep in mind, when taking melatonin, you don’t take it when you have heartburn symptoms. Melatonin should only be taken in the evening before sleep. In cases of heartburn, studies had patients take melatonin every night at bedtime (Kandil 2010).
Conclusion
GERD is a common problem often requiring treatment. Standard approaches may relieve symptoms but carry some potentially concerning long-term side effects. Dietary changes and supplements may have a place in safely eliminating symptoms in a subset of patients struggling with acid reflux symptoms.