Are Root Canals A Health Risk?
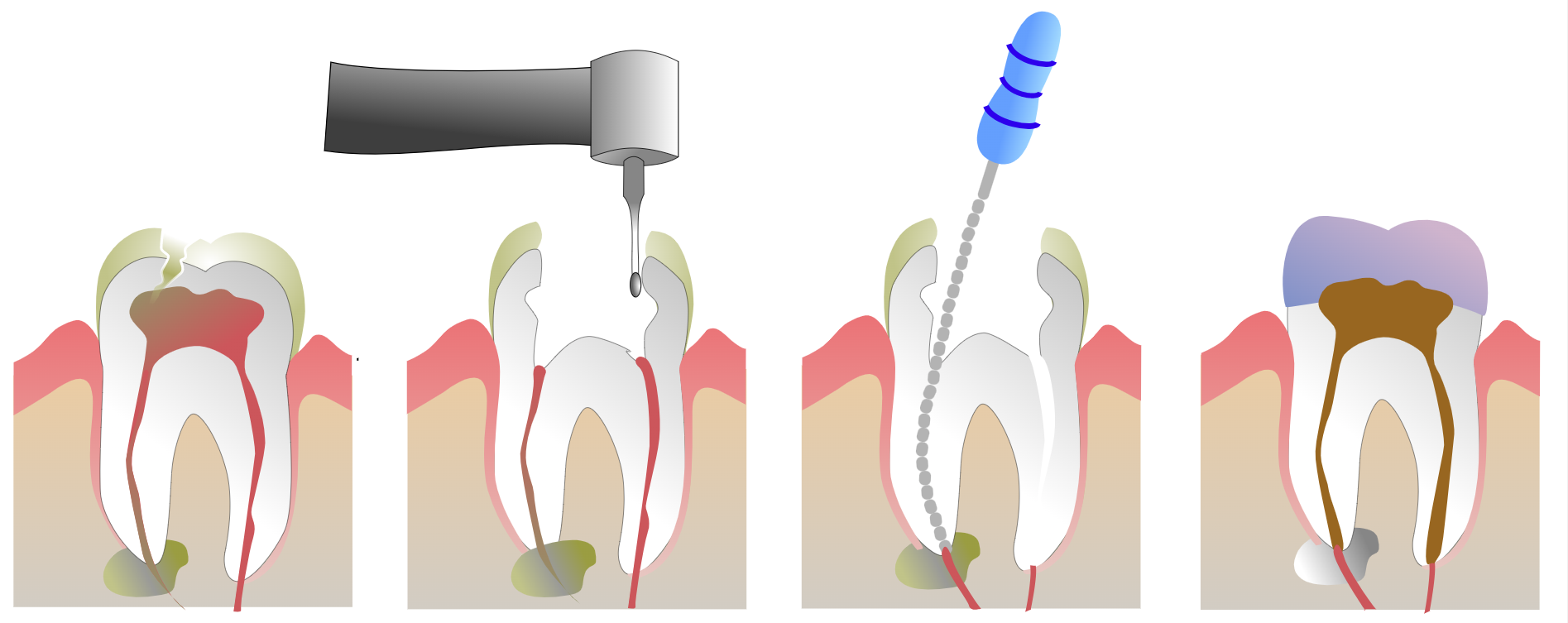
Ever since the original research by Weston Price in the 1920s, there has been controversy in alternative medicine circles around the safety of root canals. Weston Price was a dentist and researcher, well respected in his time, who explored the connection of root canal infections and chronic disease. In his research, Weston Price would remove root-canal-treated teeth from patients with chronic diseases and then implant them under the skin of test rabbits. In many cases, the rabbit would begin to display the same chronic illness as the individual from which the tooth had been removed. As such, Weston Price came to the conclusion that residual bacterial infections in root-canal-treated teeth were causing systemic illness in patients who had received root canal treatments. This hypothesis was known as focal infection theory.
The History of Focal Infection Theory
From the 1920s through the 1950s, there were numerous researchers who believed that chronic infections in the mouth, often associated with root canals or infected tonsils, were causing or contributing to arthritis, kidney problems and heart disease among other health conditions. Unfortunately, most of the clinical studies were crude, without controls and didn’t utilize appropriate techniques to minimize bacterial contamination when culturing clinical samples taken from the mouth (Murray 2000). For a more in-depth overview of the history of focal infection theory, a well-written review is available online here.
Infection Risks During Root Canal Treatment
It is well established that there is a release of bacteria into the bloodstream during root canal treatment. For susceptible patients with poor immune function, heart issues or joint replacements, oral surgical procedures—including root canals—increase the risks for infections. Research suggests that between one-third and one-half of root canals result in infectious organisms being released into the bloodstream which could cause problems in susceptible patients (Debelian 1998). However, these risks are not isolated to root canal treatment. Other research has found that tooth extractions and even just toothbrushing causes a transient increase in bacteria in the bloodstream (Lockhart 2008). As such, for any patient requiring treatment of an infected tooth, all of the available treatments will cause a transient risk of infection.
Long-Term Risks
So the question then becomes whether or not root canals can act as an ongoing source of bacteria or bacterial toxins that can have an impact on an individual’s overall health long term. While different from root canals, gum disease (periodontitis) is an infection and inflammation of the gum tissues around the teeth. Of interest, gum disease does have a negative impact on numerous health conditions.
Some of the latest research supports a strong link between gum disease and rheumatoid arthritis, heart disease and kidney disease (Molon 2019, Maddi 2013, Wahid 2013). These are the conditions that the early researchers of focal infection theory had also linked to root canals. It would not be surprising if patients that needed root canals in the early 1900s also had significant gum disease. It’s also possible that root canal infections could contain similar bacteria and bacterial toxins to infections seen in gum disease, also contributing to these health conditions. There are a couple of studies from the 1970s and 1980s that support this possibility (Dahlen 1982, Steffen 1976).
Specific Disease Relationships
Root Canals and Rheumatoid Arthritis
For rheumatoid arthritis, research suggesting a link between root canals as a contributing factor is somewhat weak. A study from 2017 looked at root canals and root canal cysts in patients with rheumatoid arthritis versus controls. While there was a slight increase in both for rheumatoid arthritis patients, the differences were not statistically significant (Jalali 2017). The minimal data available does not suggest a strong relationship between root canals and rheumatoid arthritis.
Rheumatoid Arthritis and Dental Infections: A Case Report
A case study of a patient who achieved long-term remission of rheumatoid arthritis after the removal of four diseased teeth, including one with a root canal, highlights that some rare cases may still have a significant association (Breebaart 2002). The case was unusual, as the patient had a family history of joint pain related to dental problems. In the patient’s case, he could reliably reproduce severe rheumatoid arthritis symptoms by strong pressure on the root-canal-treated tooth. Pressure was applied either by chewing hard foods like nuts and raw carrots or just with his finger. While upon visual observation, the tooth appeared unproblematic, based on his symptoms, the patient insisted on its removal.
When removed, the root canal treated tooth had an odd covering of puss, likely a bacterial biofilm, a potential source of bacterial toxins. Immediately after treatment, the patient’s arthritis symptoms again flared up, but then went into remission for around four months. With the resurgence of symptoms, the patient discovered an additional three teeth that were loose that could also cause arthritis symptoms when pressed with his finger. Once these additional three teeth were removed, the individual became completely free of rheumatoid arthritis symptoms for the next 16 years.
While fascinating, this individual case does not demonstrate how common this relationship could be. Considering there don’t appear to be any other similar case reports, it’s likely fairly uncommon.
Root Canals and Heart Disease
Unfinished Root Canals
For the link between heart disease and root canals, one study looked at the worst case scenario: unfinished root canals and their relationship to heart disease (Lin 2015). Unfinished root canals are where the tooth was drilled out but the root canal was never filled and completed. These patients should be at a very high risk for chronic root-canal infections since the tooth had never been properly treated and filled. If there is any possible relationship between a root canal and heart disease risk, unfinished root canals are almost the perfect model to identify significant problems.
In the study, one or two unfinished root canals increased the risk for heart disease by 22%. For three or more unfinished root canals, the risk increased dramatically by 261%. While any increased risk is concerning, to put the risk in perspective, smoking increases the risk of high-blood-pressure-related heart disease by 240% (Carter 2015). Also keep in mind that most root canals are “finished,” so real world risks would be significantly lower for most individuals.
Normal, Finished Root Canals
A separate study looking at finished root canals and heart disease found a modest association. The data on over 30,000 male health professionals found that dentists had a 21% increased risk of heart disease from one or more root canals. Yet oddly, the findings did not extend to other health professions (Joshipura 2006).
A study on over 15,000 individuals exploring both the self-reporting of root canals and heart disease found a 37% increased risk with one root canal and a 62% increased risk for two root canals for individuals who still had 25 or more teeth (Caplan 2009). While interesting, self-report studies are subject to misinterpretations and bias from the study subjects. An earlier study on over 1000 Swedish women found no association between root canals and heart disease, heart attack and angina, a type of chest pain related to heart disease (Frisk 2003).
In 2020, a research group assembled all the available evidence on “apical periodontitis”—the term for root canal infections—and heart disease risk. The researchers found a weak association between the two, but the quality of the evidence was moderate to low (Jakovljevic 2020).
Conclusion
Based on the available evidence, it appears that root canals may, when finished properly, have a small negative impact on health. This relationship is most likely associated with heart disease but could also extend to other inflammatory conditions like rheumatoid arthritis. However, more research of better quality is needed to fully validate the existence and strength of the association. The idea that root canals are a major detriment to overall health appears unlikely from the available research. Still, there may be specific situations where a root canal is of poor quality or the treated tooth becomes reinfected. In these situations, the root canal still needs appropriate follow-up treatment.



