Osteoarthritis: A Brief Review of Integrative Treatment
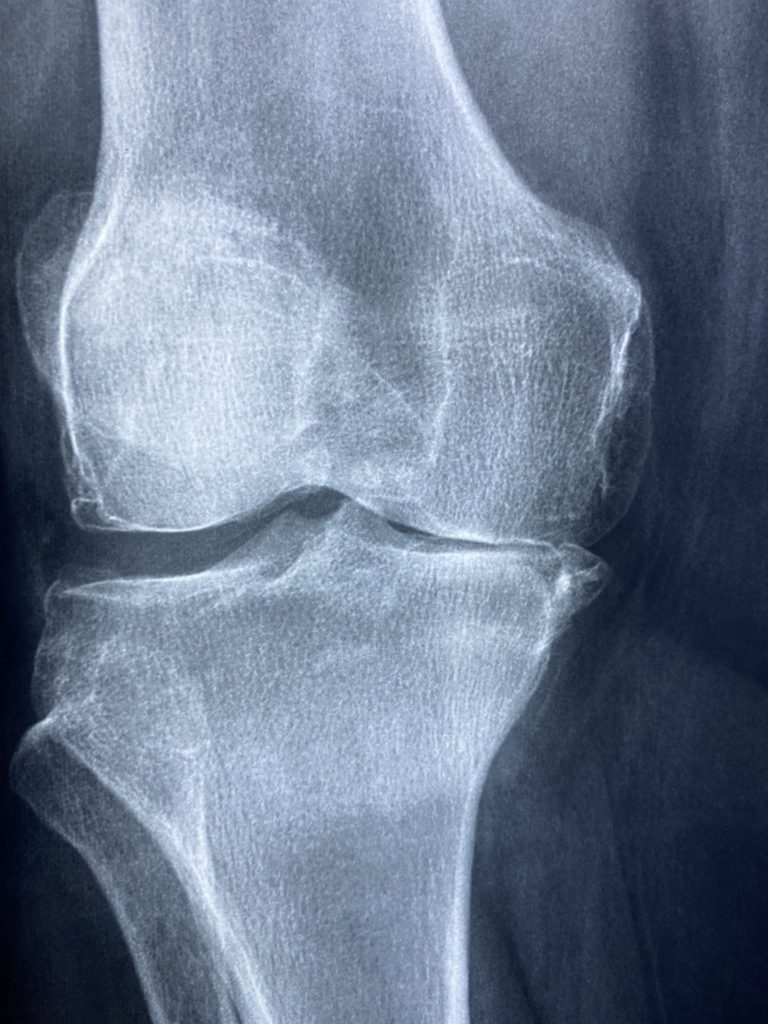
Osteoarthritis is generally considered wear and tear from overuse of a joint. Overtime, cartilage—which acts as a protective cushion—can wear down causing or contributing to pain. However, it’s worth recognizing that this is a vast oversimplification of the condition. While mainstream Western medicine often focuses on the physical aspects of the disease, imaging studies call this understanding into serious question.
Even some of the earliest research on the prevalence and associations of joint wear and tear showed startling discrepancies. First noted in the early 1960s, in a sample of men and women with advanced osteoarthritis seen on X-ray, only 40% of men and 50% of women reported any current symptoms of arthritis (McAlindon 1999). Additional studies have largely confirmed these findings (Gresham 1975). It has been obvious for years that damage to the joint does not always create pain and dysfunction. So the question obviously arises, why is there pain in some patients, but not in others?
Pain in Osteoarthritis
While a number of factors play a role, local inflammation often with increased pressure within the joint can lead to pain (Nees 2019, Carlesso 2019). Of interest, individuals with pain from osteoarthritis seem to be particularly sensitive to increased pressure. In addition, changes in the brain itself appear to have a role. Increased brain sensitivity and activation are often present, likely contributing to chronic pain symptoms (Fingleton 2015).
Chronic pain in osteoarthritis is associated with what is medically termed allodynia. Allodynia is a pain response to a situation or stimulus that is typically not painful. In a sense, the brain is misinterpreting signals from the joint. This kind of situation often makes people erroneously conclude that the person is “faking” the pain, or that it’s “all in their head”. However, allodynia is not under conscious control. It’s possible that even individuals with severe damage may be able to improve and minimize pain if they can address and reverse inflammation and pain sensitization in the brain.
Mental Health and Osteoarthritis
In osteoarthritis, negative mental health outcomes—including depression and anxiety—have consistently been linked to poor outcomes and disability (Baar 1998). Pain and pain flares have significant links to mental health as well (Wise 2010). Improvements in depression have also been shown to improve osteoarthritis pain and functional ability (Lin 2003). In patients with more severe osteoarthritis, mental health needs to be addressed appropriately.
Erroneous belief patterns that affect long-term recovery are common in osteoarthritis. Pain is often unpredictable and becomes associated with use. As such, patients often get trapped in “fear avoidance” and anxiety about their condition (Scopaz 2009). This leads to decreased activity and exercise. Over time, decreased use can make the condition worse.
While you don’t want to discount pain, you do want to encourage use of the joint as appropriate. Moderate exercise is well-known to help decrease pain and improve function in osteoarthritis. Done properly, it also has a large margin of safety with minimal side effects (Wellsandt 2018). Proper exercise should be the foundation of most strategies to help osteoarthritis symptom improvement. Beyond standard exercise, yoga, tai chi and qigong are all options with evidence for benefits, although more research is needed (Lauche 2019, Huston 2016, Zeng 2020).
Risk Factors
Risk factors for osteoarthritis include (Pereira 2015):
- Older age
- Female gender
- Excessive use of a joint or joints
- Being overweight
- Poor nutrition
Some risk factors for osteoarthritis can be modified to improve outcomes. Losing weight can decrease strain on joints. In addition, obesity is well known to be associated with low-level inflammation, likely worsening arthritis and pain (Berenbaum 2013).
If a certain activity is putting excessive strain on a joint, modifying or eliminating the activity may become necessary. Jobs that are physically demanding or involve repetitive motions often have increased rates of osteoarthritis.
In addition, poor nutrition should be addressed. Eating a healthy diet appears to decrease risks of chronic inflammation and arthritis (Messina 2019). Deficiencies in vitamin C and vitamin D also may lead to progression of the disease (Wang 2017, Wang 2004).
Supplements for Osteoarthritis

Evidence from research on dietary supplements has shown potential, although research quality is often poor. The supplements with the strongest evidence for significant pain reduction include:
- Curcumin
- Boswellia
- Pycnogenol
- And others…
Curcumin is the yellow pigment found in turmeric. For osteoarthritis, curcumin appears to have promise for reducing symptoms. I’ve covered research on curcumin previously here.
Boswellia is commonly known as frankincense. It also appears to have significant anti-inflammatory effects that may be useful in decreasing the pain and inflammation seen in osteoarthritis. A recent meta-analysis concluded that both curcumin and boswellia appear quite promising for treatment with low risks for side effects (Bannuru 2018).
Pycnogenol is the trademarked name of a French pine bark extract. Studies have been continuing to find interesting clinical benefits with this anti-oxidant and anti-inflammatory compound. For osteoarthritis, it has been shown to yield benefits in clinical studies and appears to arrest joint destruction (Rohdewald 2018).
Other treatments may potentially hold promise, including ginger, l-carnitine, collagen and green-lipped mussel extract (Liu 2018, Altman 2001).
Conclusion
Osteoarthritis is often a chronic condition that can lead to significant decreases in the quality of life. Standard treatments are not curative and alternative approaches are worth considering. The latest evidence suggests the disease is multifactorial, and addressing patients’ mental health and beliefs, nutritional factors and exercise can yield significant benefits. In addition, a number of supplements show early promise for helping decrease symptoms and potentially slowing progression of the disease.



Im grateful for the blog article. Thanks Again. Much obliged.
Wow, great article post.Really thank you! Will read on…
There’s certainly a great deal to learn about this topic. I love all of the points you made.
Thank you for sharing your thoughts. I truly appreciate your efforts and I will be waiting for your further post thank you once again.